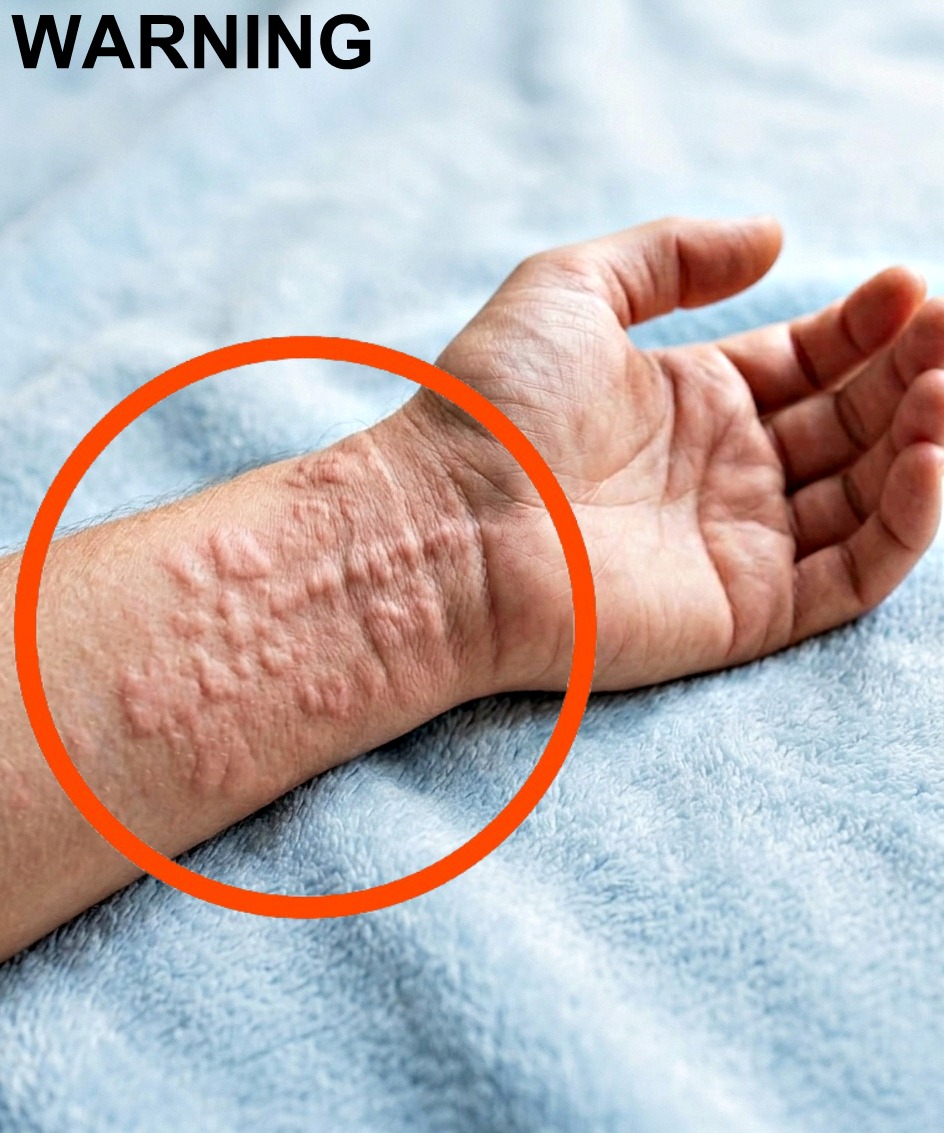
Skin that suddenly burns, swells, or erupts into hives may look at first like “just an allergic reaction.” But when those symptoms arrive alongside breathing trouble, chest tightness, dizziness, or swelling around the face and throat, the situation can become life-threatening frighteningly fast. What begins as itching or redness can escalate within minutes into Anaphylaxis — a severe, whole-body allergic reaction capable of shutting down breathing and circulation if not treated immediately.
That is what makes anaphylaxis so dangerous: people often underestimate the moment when discomfort turns into emergency.
A rash alone can be unpleasant but manageable. Hives, itching, and redness happen for many reasons and are often harmless. But when the body’s reaction spreads beyond the skin and begins affecting breathing, blood pressure, or swelling in the airway, the immune system is no longer simply irritated — it is overreacting violently. During anaphylaxis, the body releases large amounts of chemicals that can cause airways to narrow, blood vessels to dilate dangerously, and tissues to swell rapidly. The result can feel terrifying: wheezing, tightness in the chest, difficulty swallowing, swollen lips or tongue, nausea, vomiting, confusion, faintness, or a racing heartbeat.
People experiencing it sometimes describe the sensation as their body suddenly “turning against itself.”
The triggers can vary widely. Foods such as peanuts, shellfish, milk, eggs, or tree nuts are common causes. Medications including antibiotics or pain relievers can also provoke severe reactions. Insect stings, latex exposure, or even exercise combined with certain foods may trigger anaphylaxis in some individuals. Sometimes, despite extensive testing, the exact trigger remains unknown. That unpredictability is part of what makes severe allergic reactions emotionally frightening for both patients and families.
One of the most dangerous mistakes people make is waiting too long to act because they hope symptoms will settle on their own. Early signs can seem deceptively mild: flushing skin, itching, tingling, mild swelling, or stomach discomfort. But anaphylaxis can accelerate rapidly, and once breathing becomes affected, every minute matters. Swelling inside the throat may worsen suddenly, making it harder to speak, swallow, or inhale enough air. Blood pressure can drop sharply, leading to collapse or shock.
That is why medical experts stress one message repeatedly: if a rash appears together with breathing problems or swelling around the face and throat, treat it as an emergency immediately.
The first-line treatment for anaphylaxis is epinephrine, commonly delivered through an auto-injector such as an EpiPen. Epinephrine works quickly to relax airway muscles, tighten blood vessels, reduce swelling, and help stabilize the body before the reaction progresses further. Many people hesitate to use it because they fear overreacting or giving medication unnecessarily. But doctors consistently emphasize that delaying epinephrine during a severe allergic reaction is far riskier than using it too early.
Emergency services should always be called after epinephrine is administered because symptoms can sometimes return even after initial improvement. Medical monitoring remains important, especially in severe reactions involving breathing difficulty or low blood pressure.
While waiting for help, keeping the person lying down if possible can help maintain blood flow and reduce the risk of collapse. Tight clothing should be loosened, and breathing monitored carefully. If vomiting occurs or breathing becomes difficult while lying flat, repositioning safely on the side may help. Above all, the person should never be left alone during anaphylaxis because conditions can worsen suddenly.
Stories of severe allergic reactions often stay with people because of how quickly ordinary moments can transform into medical emergencies. A meal at a restaurant. A bee sting during a picnic. A new medication taken before bed. One moment life feels completely normal; minutes later, someone is struggling to breathe. The speed of the transition shocks many people who previously associated allergies only with sneezing, mild rashes, or seasonal discomfort.
Awareness matters because recognizing the pattern early saves lives. The body gives warning signs before collapse happens: hives spreading rapidly, swelling around the eyes or mouth, wheezing, dizziness, sudden weakness, or a sense that “something is very wrong.” Trusting those signals and acting immediately can prevent tragedy.
At the same time, living with severe allergies often creates emotional burdens outsiders rarely see. People with known anaphylactic allergies frequently move through life with constant vigilance — checking food labels repeatedly, asking restaurant questions others never think about, carrying emergency medication everywhere, and quietly calculating risk in everyday situations. Families of children with severe allergies especially understand how quickly fear can enter ordinary routines.
In the end, the most important truth about Anaphylaxis is that it is both terrifying and treatable when recognized quickly. A rash combined with breathing difficulty is not something to “wait out” casually. It is the body sounding an alarm that something much more serious may already be unfolding internally.
And sometimes, recognizing that alarm early — before panic, before collapse, before the airway closes further — becomes the difference between a frightening emergency and a life that can still be saved.