The burning sensation often begins without warning. It doesn’t arrive with a clear cause or an obvious trigger—just a strange discomfort that feels out of place. At first, it might seem minor: a patch of skin that feels unusually sensitive, a dull ache that doesn’t quite make sense, a fatigue that lingers without explanation. It’s easy to dismiss these early signs, to assume they’re temporary or unrelated. But over the next few days, something changes.
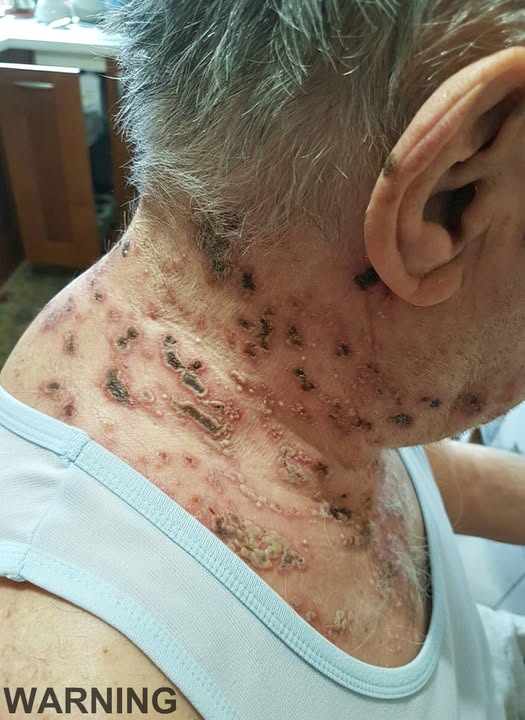
Then the rash appears.
By that point, the situation can feel entirely different. What started as a vague discomfort can intensify into pain that is sharp, persistent, and difficult to ignore. For many, this is the moment when concern replaces uncertainty. Yet one of the most common misunderstandings about this condition is who it affects. There’s a widespread belief that shingles only occurs in people who are already very ill or significantly older. In reality, the risk is far broader—and the reason lies in something most people don’t realize: the cause has been present in the body for years.
Shingles is linked to the same virus that causes Chickenpox, known medically as the Varicella-zoster virus. After someone recovers from chickenpox, the virus doesn’t fully leave the body. Instead, it remains inactive, hidden within the nervous system. It can stay there silently for decades, causing no symptoms and giving no indication that it’s still present.
Under certain conditions, however, the virus can reactivate. This doesn’t happen randomly—it is often associated with changes in the immune system. Factors such as aging, prolonged stress, illness, or periods of physical and emotional exhaustion can reduce the body’s ability to keep the virus in its dormant state. When that balance shifts, the virus can begin to travel along nerve pathways, leading to the symptoms associated with shingles.
The early stage can be difficult to recognize. The sensations—burning, tingling, stabbing pain—are often localized to one specific area of the body. Because they occur before any visible signs, they are frequently mistaken for muscle strain, minor injury, or general fatigue. It is only later, when the rash develops, that the pattern becomes clearer.
The rash itself typically follows the path of a nerve, appearing on one side of the body or face. It may begin as redness and small blisters, gradually becoming more noticeable. While the skin changes are often the most visible part of the condition, they are not always the most significant. For many, the pain associated with the nerve involvement is the most challenging aspect.
In some cases, even after the rash fades and the skin begins to heal, the pain does not fully go away. This can lead to a condition known as postherpetic neuralgia, where nerve pain persists for an extended period—sometimes months or longer. This type of pain can vary in intensity, but it is often described as ongoing and disruptive, affecting daily activities, sleep, and overall well-being.
Another important aspect to understand is how shingles relates to others. While shingles itself is not spread from person to person in the same way as many infections, the underlying virus can still be transmitted. If someone who has never had chickenpox—or has not been vaccinated—comes into contact with the fluid from shingles blisters, they may develop chickenpox rather than shingles. This makes awareness and precaution important, especially around vulnerable individuals.
Prevention and early response play a key role in managing the condition. Vaccination is one of the most effective ways to reduce the risk, particularly for those in higher-risk groups. Maintaining overall health—through balanced nutrition, rest, and stress management—can also support the immune system’s ability to keep the virus inactive.
Equally important is recognizing the early signs. When symptoms appear that feel unusual—especially localized pain or sensitivity that doesn’t have a clear cause—it is worth paying attention. Seeking medical advice early can lead to timely treatment, including antiviral medications that may reduce the severity and duration of the condition.
What makes shingles particularly challenging is how quietly it begins. The initial signals are easy to overlook, easy to explain away. But those early moments are often the most important.
Because the body often gives subtle warnings first.
And listening to those warnings—before they intensify—can make a meaningful difference in how the experience unfolds