Sex can quietly shift from intimacy into pain in ways many people never expect.
Not because of shame.
Not because of recklessness.
And not because anyone necessarily did something “wrong.”
Sometimes, what begins as warmth, closeness, affection, and physical connection slowly turns into burning discomfort that appears days later without warning. A strange ache in the bladder. A constant urge to urinate even when almost nothing comes out. A sharp, stinging sensation that makes every trip to the bathroom feel unbearable.
For many women especially, the experience feels confusing at first.
The symptoms seem to appear out of nowhere.
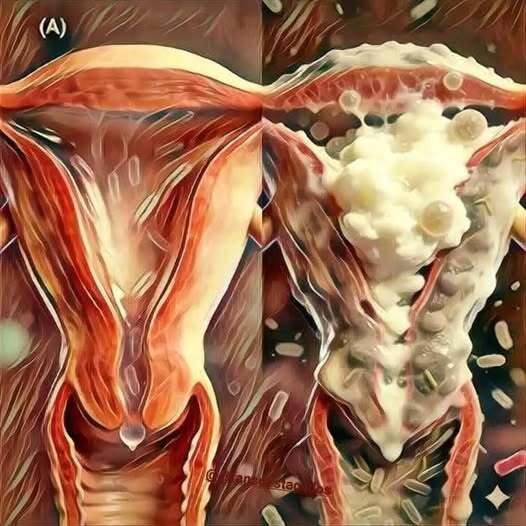
But often, the cause is connected directly to the body’s anatomy and how sexual activity affects the urinary system.
Most people are never taught just how physically interconnected intimacy and urinary health actually are. During sex, friction, warmth, moisture, and close skin contact create conditions that make it easier for bacteria — particularly bacteria naturally found around the genital and anal areas — to travel toward the urethra, the small tube that carries urine out of the body.
Because women have a much shorter urethra located close to both the vagina and anus, bacteria can reach the bladder more easily than in men. Once bacteria enter the urinary tract, they can multiply rapidly, triggering a urinary tract infection, commonly called a UTI.
And despite how common these infections are, many people still feel embarrassed discussing them openly.
That silence often makes the experience feel isolating.
Women sometimes blame themselves, believing poor hygiene, sexual behavior, or personal failure caused the infection. In reality, even careful hygiene, consensual sex, and healthy relationships do not eliminate the risk completely. Some bodies are simply more vulnerable than others due to anatomy, hormones, hydration levels, friction, or individual bacterial sensitivity.
What begins as mild irritation can quickly become physically exhausting.
Burning urination.
Pelvic pressure.
Cloudy or unusually strong-smelling urine.
Persistent urgency.
Pain that lingers long after intimacy ends.
And when infections become recurrent, the emotional effects can grow just as heavy as the physical symptoms. Many women begin feeling anxious before intimacy itself, worried the cycle will repeat again. Some avoid closeness entirely out of fear. Relationships can quietly absorb tension nobody expected because something once associated with comfort and connection has become linked to discomfort and dread.
That emotional layer is rarely discussed enough.
Because recurring UTIs are not just medical inconveniences.
They can slowly erode confidence, spontaneity, relaxation, and trust in one’s own body.
The good news is that small habits can dramatically reduce the risk for many people.
One of the most recommended preventive steps is urinating soon after sex, which helps flush bacteria away from the urethra before they can travel upward into the bladder. Staying well hydrated also matters because frequent urination naturally helps clear bacteria from the urinary tract throughout the day.
Other supportive habits include using adequate lubrication during intercourse to reduce friction, wearing breathable cotton underwear, avoiding prolonged damp clothing, and staying away from harsh soaps, heavily scented products, or douches that can disrupt the body’s natural protective balance.
For people experiencing frequent infections, medical evaluation can also be important. Sometimes recurring UTIs are connected to hormonal changes, underlying conditions, or bacterial resistance that may require professional treatment or preventive strategies.
Most importantly, awareness removes unnecessary shame.
These infections are incredibly common.
They do not make someone “unclean,” irresponsible, or broken.
They are often the result of ordinary biology interacting with intimacy in ways many people simply were never taught to understand.
And perhaps that understanding matters more than people realize.
Because intimacy should not leave someone quietly suffering days later, afraid to explain why they suddenly seem uncomfortable, withdrawn, or anxious.
With education, communication, and a few practical precautions, sexual connection can remain what it was meant to be:
Safe.
Tender.
Comforting.
And free from the silent pain too many people endure without ever talking about it.